This story was written by Charles, heart and kidney recipient.
My name is Charles Cook. I am 53 years old. I am the father of 2 fantastic young adults. I am a 2 time deceased donor organ transplant recipient. I received my heart in April 2016 and I received my kidney in October 2017. I was born and raised in the Great State of Georgia but I have called the province of Ontario Canada my home since the summer of 2006. The following part of my story covers my heart transplant journey.
Besides a love for playing in red clay and eating peaches, I was also born with a heart condition called Hypertrophic Cardiomyopathy. My heart condition went undetected until I was 17 years old. I graduated high school that same year. That particular summer I attended what 1500 of my classmates and I liked to call Camp Tecumseh. The rest of the world referred to it as Plebe Summer at the United States Naval Academy.
 Plebe Summer was sort of like our boot camp. I had played football, wrestled, and ran track in high school, so I was in excellent physical condition when I arrived at the academy. I made it through the physical part of the summer with no problem. Before the summer ended I had earned the right to wear the jersey of a Super Mid.
Plebe Summer was sort of like our boot camp. I had played football, wrestled, and ran track in high school, so I was in excellent physical condition when I arrived at the academy. I made it through the physical part of the summer with no problem. Before the summer ended I had earned the right to wear the jersey of a Super Mid.
We started the academic year that fall after the upperclassmen returned from Summer Leave. At the end of the first week of classes our company went for a run. I started off up front in my normal spot with the leaders. Then I started getting chest pains which caused me to slow down my pace until I was at the back of the pack. One of my upperclassmen asked me what was wrong with me. I didn’t have an answer because I had never experienced anything like that before. He told me to knock it off and call it a day.
The following week I tried running again after class on 2 separate occasions. The chest pains returned each time. I went back to my upperclassmen to let them know what was going on. I was told to go down to the clinic to get myself checked out.
I went to the clinic as ordered and I received a very thorough physical examination. My test results came back requiring further testing. That was the beginning of the end of my naval career, I just didn’t know it yet. I did more tests at the hospital on base and then I was sent to Bethesda Naval Hospital for even more tests. I was seen by the Chief Cardiac Surgeon of The Navy who diagnosed me with HCM, a heart condition that caused the muscles in the walls of my heart to grow to become abnormally thick. Eventually my heart muscles could grow so thick that they would lose their ability to contract properly and I could die.
Once I had my diagnosis the only question remaining unanswered was when I would have to leave the academy. I was allowed to finish out my first semester of classes. Then I went home for Christmas Leave in December without having received a final decision about my official last day. Due to a mix up in the lines of communication I returned to the academy in January to begin my second semester.
I found out 2 weeks later from my Company Officer that the decision had been made that I was to receive a medical separation from the academy. I was supposed to have been informed of the decision while I was at home for Christmas but somehow word had never made it to me. My career as a midshipman was over and I didn’t have a clue about what I was supposed to do next.
 Fast forward 18 years. After things hadn’t worked out with my plans to become a great naval officer I found my next path and passion in the restaurant business. I started off as a dishwasher at age 19. I worked my way through school holding just about every position found within the 4 walls of a restaurant except for owner and manager. I eventually achieved a B.S. degree in Hotel/Restaurant Management from Florida International University. It was the 5th institution of higher learning that I had attended since graduating high school.
Fast forward 18 years. After things hadn’t worked out with my plans to become a great naval officer I found my next path and passion in the restaurant business. I started off as a dishwasher at age 19. I worked my way through school holding just about every position found within the 4 walls of a restaurant except for owner and manager. I eventually achieved a B.S. degree in Hotel/Restaurant Management from Florida International University. It was the 5th institution of higher learning that I had attended since graduating high school.
At the age of 36 I was the Regional Employment Manager for the Atlanta Region of the Longhorn Steakhouse Division of RARE Hospitality International Incorporated. Try saying that 3 times fast. I was responsible for the management staffing for 40 restaurants in Metro Atlanta. I loved my job. I was married with 2 beautiful young children. I hadn’t had a single HCM related issue since I had left Annapolis. Life was good!
Then things changed. I was driving home from work after spending the day interviewing potential management candidates at our restaurant in Athens. I had just gotten on the highway when out of nowhere I suffered a massive right brain ischemic stroke. The entire left side of my body was wiped out. It took 14 months of rehab and recovery to put me back together again. The neurologists said that I had too much residual brain damage to return to my old job. I tried anyway and I found out that they were right. My career in restaurant management was over. I think that I might be detecting a pattern.
Once the doctors cleared me to travel, our family relocated to southwestern Ontario, Canada. We knew that my stroke was just the beginning of the very bad stuff that could happen because of my HCM. My first cardiologist in Canada reinforced that knowledge when he told me that there was no cure for HCM and it never got any better. I went into end stage heart failure 3 years later. The same cardiologist told me that there were only 3 outcomes with heart failure: artificial heart, heart transplant or death. He was right, and I experienced all 3!
While I was in the early days of end stage heart failure my local cardiologist began sending me to Toronto General Hospital (TGH) to be monitored because they did the heavy lifting on that type of heart condition. Since we knew where I was headed my cardiologist thought that it would be a good idea for TGH to develop a patient history with me before my condition got any worse. I was monitored by my local cardiologist and the Heart Function Team at TGH for nearly 6 years all the while waiting for the other shoe to drop on my heart health.
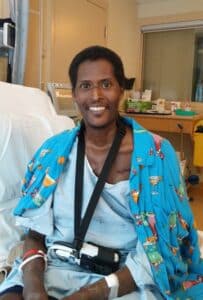 The bottom finally fell out in January 2015 when I went to Toronto General Hospital for a regular check up and I didn’t get to go home for 100 days. I did a stress test which showed that my heart had worn out to the point that I needed a heart transplant. I did another test which showed that there was so much pressure built up inside my chest that it was unsafe for me to receive a heart transplant at that time. The team decided that the best thing to do would be to give my heart a helper in the form of a mechanical pump called a Left Ventricular Assist Device (LVAD).
The bottom finally fell out in January 2015 when I went to Toronto General Hospital for a regular check up and I didn’t get to go home for 100 days. I did a stress test which showed that my heart had worn out to the point that I needed a heart transplant. I did another test which showed that there was so much pressure built up inside my chest that it was unsafe for me to receive a heart transplant at that time. The team decided that the best thing to do would be to give my heart a helper in the form of a mechanical pump called a Left Ventricular Assist Device (LVAD).
The LVAD surgery saved my life but it cost me my kidney function. Several complications arose during surgery including me dying twice on the table and being brought back to life through the use of cardiac massage. I lost a lot of blood and my kidneys ran dry for too long and they wound up dying. Immediately after surgery my doctors hoped that a boost from hemodialysis might wake up my dormant kidneys but that never happened. I remained on hemodialysis from the day of my surgery until the day I received my kidney transplant well over 2,5 years later. Before I had my surgery I hadn’t even known that my kidneys were at risk. That made me angry!
After spending exactly 100 days at TGH I was finally discharged. I went home for 3 weeks and then I had to come back to the hospital and undergo a second LVAD surgery in order to replace my original LVAD. While I was at home my blood work showed a large increase in the level of a substance called LDH. LDH is created when large amounts of red blood cells get broken down at one time. When my original LVAD was removed and examined a large mass of broken down red cells was found inside just waiting to gum up the inner workings of the pump. If it hadn’t been caught when it was I probably wouldn’t be writing this story because I would have been dead.
My second LVAD surgery went great without any major complications. I was discharged after only 36 days! That beat 100 days by a mile. The pressure test was redone 3 months after my surgery. The results were within range making me eligible to be placed on the transplant waiting list for my heart. I was told at that time that I could expect to wait 2-3 years for a heart because of my O+ blood type. I had no problem waiting. I was glad to be alive and I figured that it would probably take at least 2-3 years before my brain could begin to fully process everything that had happened in the previous few months.
When I returned home I became the first LVAD in-center hemodialysis patient that my local hospital had ever treated. It was a learning experience for everyone involved. With a lot of education, good communication and teamwork the dialysis staff and I found a way to make it work. Things were going so well that somewhere around the 10 month mark of my in-center dialysis treatments, one of the doctors at TGH suggested that I might be a great candidate to be trained to do hemodialysis at home. Say what?!
I thought that the whole home hemodialysis plan might have been asking a bit too much. I was just getting comfortable with living with a heart that ran on batteries during the day. At night I plugged myself into the wall like a lamp so that I could sleep for longer than the 5 hours of energy that the batteries provided. I was not a big fan of the idea at first. I eventually grew to dislike my in-center hemodialysis schedule enough to be willing to try something different. I wound up feeling like a wrung out dish rag after each of my runs with zero energy to do anything but fall asleep on the couch. I needed something to change.
Despite my initial skepticism towards my readiness for the challenge, I entered the Home Hemodialysis training program. After 5 successful weeks of training I was told by the training nurses that they were planning for me to begin doing my runs at home the following week. I received this news on a Friday morning and by that point in my training I felt that I was capable of performing a dialysis run safely on my own. In order to make sure that nothing fell through the cracks I was instructed to return to the training room the following Monday morning for my final check run. If that went well then a dialysis machine would be delivered to my home. The following day one of the training nurses would sit with me as I did my first run at home. If that went well then I would start my solo home hemo career the next day. After I finished my run in the training room I wished everyone a good weekend and I went home excited to tell my new wife Monica the good news,
The next morning Monica left for work. The phone rang and when I answered it I heard the voice of a Transplant Coordinator from TGH. She told me that they thought that they had a heart for me and that I needed to get down to the hospital as quickly and safely as possible. I hung up the phone and I immediately dialed I Monica’s work number. I had to leave a message with the receptionist asking that Monica call me back as soon as she could because it was literally a matter of life and death. When Monica called me back I told her that I had just gotten The Call.
Monica returned home and we were out of the door in a flash bound for TGH. She reminded me months later that I was the one who drove us to the hospital.. I had completely forgotten that little detail along with many others from that wonderfully unexpected day. By the time that we got on the road I had thoroughly convinced myself that there was no way that a heart had been found for me in only 9 months after getting listed when I had been told that I would be waiting at least 2-3 years.
I was prepared to experience what’s called a dress rehearsal. That’s a situation where you get the call that an organ may be available for you but when you get to the hospital it turns out that it’s not the right match and you go home without your new organ. That is what I was prepared for. What I wasn’t prepared for was for everything to go through on the first try which it did.
 I still can’t remember anything after checking in at admissions until I woke up in my recovery room with someone else’s heart in my chest. I remember opening my eyes for the first time after surgery. I looked up at the ceiling and around at the window and the walls. I remember thinking I’m alive! Thank you God! You got me through another one! Then I remember thinking that I’m alive because I have someone else’s heart in my chest. I had never felt so thankful, so humble and so unworthy all at the same time. I couldn’t think of a single thing that I had ever done in my life that made me worthy to receive such a precious gift. I broke down and I cried like a baby.
I still can’t remember anything after checking in at admissions until I woke up in my recovery room with someone else’s heart in my chest. I remember opening my eyes for the first time after surgery. I looked up at the ceiling and around at the window and the walls. I remember thinking I’m alive! Thank you God! You got me through another one! Then I remember thinking that I’m alive because I have someone else’s heart in my chest. I had never felt so thankful, so humble and so unworthy all at the same time. I couldn’t think of a single thing that I had ever done in my life that made me worthy to receive such a precious gift. I broke down and I cried like a baby.
I remained in that same mental state for weeks afterwards and I had the same reaction each time I thought of my new heart and my unworthiness to receive it. Why did I get a heart when so many other people didn’t who were just as if not more deserving than I was? I finally came up with an answer that gave me some peace of mind. One tearful night when I was unable to sleep I had a long conversation with myself in my bathroom mirror. I tried to put myself into the mindset of the person who had donated their heart. This was an individual who with their final wishes wanted to do something to help someone else have a chance at a better life. I became the beneficiary of that good will. In my case I was someone they didn’t even know. If that wasn’t paying it forward then I didn’t know what was.
 I decided to live my life in a way that honored my donor and their family by doing whatever I could to pay it forward to all of the patients coming along behind me. That brings me to the reason that I’m writing this story. I share my story now in the hope that it will benefit others. Thank you for sticking with me until the end. I’ll have to share the rest of my kidney journey another time.
I decided to live my life in a way that honored my donor and their family by doing whatever I could to pay it forward to all of the patients coming along behind me. That brings me to the reason that I’m writing this story. I share my story now in the hope that it will benefit others. Thank you for sticking with me until the end. I’ll have to share the rest of my kidney journey another time.
Organ donation can not only save lives it can also improve the quality of the lives of transplant recipients exponentially. Please consider becoming a registered organ donor. Then be sure to explain your wishes to your family.


Leave a Reply